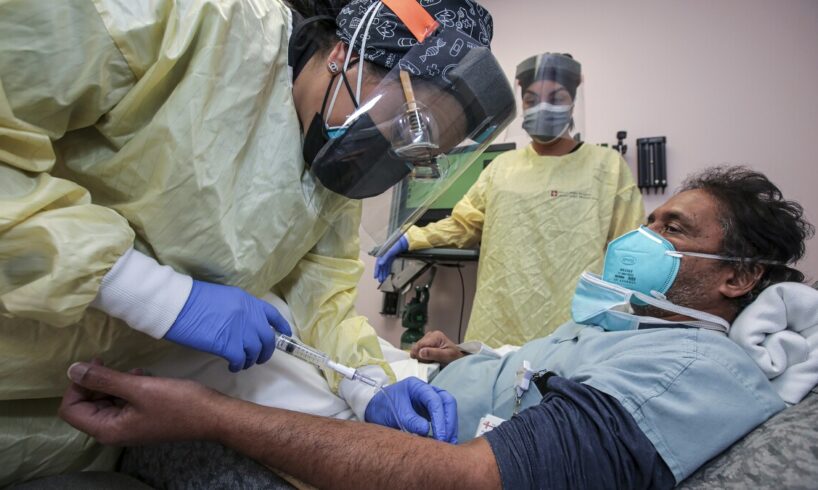
So much of the last two years has felt surreal for the staff at Centro De Salud Familiar La Fe, a federally qualified health center in El Paso. Seemingly overnight, the women’s health center became a coronavirus unit. They began offering COVID-19 testing, and then, as soon as they could, vaccine pop-ups. They’ve made public service announcements and gone door to door, encouraging people to get vaccinated.
But despite the unprecedented nature of the pandemic, some things did not come as a surprise — like how hard it hit their low-income and uninsured clients.
“This area has been hurting for a long time,” spokesperson Estela Reyes-López said. “We do not get the funding that we need. We don’t have the medical providers that we need. … The situation with the coronavirus just exacerbated things that were already happening.”
La Fe primarily serves low-income and uninsured Texans, and it has seen firsthand the disparate impact the pandemic has had on the most vulnerable communities. Many work hourly, public-facing jobs that don’t allow them to wait in line for COVID-19 tests — or take time off to quarantine. Others have chronic, untreated health conditions that make them more susceptible to severe cases of the disease. Nationally, uninsured people have lagged behind in vaccination rates.
And now, with a new COVID-19 wave threatening to crash on Texas’ shores, the staff at La Fe are once again preparing for it to hit these same communities the hardest.
“The biggest crisis we have among the uninsured right now is confusion over the cost of getting tested and where they can get the tests,” said La Fe community health administrator Jorge Salazar. “And then the vaccines, which come at no cost, but when people are not accustomed to that, they still hesitate.”
Medical vulnerabilities
A lot of questions remain about omicron, the highly contagious new coronavirus variant, but health care experts say preparation has proven key to how a community weathers the disease. And many uninsured and low-income Texans may be at a preparation deficit after decades of being medically underserved.
In 2019, more than 18% of Texans were without health insurance, the highest rate in the country and more than double the national average. Texas is one of just 12 states that opted out of expanding Medicaid access under the Affordable Care Act.
In El Paso County, where La Fe is based, about a quarter of adults under the age of 65 don’t have health insurance. Salazar said this means the area was already behind the ball when the pandemic hit.
“The problem is the historical lack of health insurance, not just the lack of health insurance now,” Salazar said. “They haven’t been able to attend to preventive care or maintain their health.”
Salazar said the health center’s clients are often dealing with chronic or untreated health conditions that compromise their immune systems and make them more vulnerable to getting a severe case of COVID-19. This undertreatment may have been exacerbated during the pandemic, he said, as many people avoided or were unable to get treatment at emergency rooms, which can be an entry point to the health care system for uninsured patients.
It’s a similar story in the Rio Grande Valley, which, like El Paso, has among the lowest rates of health insurance in the state.
“There are a lot of individuals here who have comorbidities such as undiagnosed or undertreated diabetes, as an example,” said Michael Dobbs, vice dean of clinical affairs and chief medical officer at the University of Texas Health Rio Grande Valley. “Their immune systems may not work as well. They’re more prone to infections. And so being in the hospital for a long time on a ventilator is very dangerous for those patients.”
“The perfect storm”
With the holidays looming and omicron on the rise, many Texans are scrambling to get their hands on COVID-19 tests. But that, too, will be harder for low-income and uninsured Texans, many of whom won’t be able to afford expensive at-home kits or wait in long lines at free testing sites.
“In the beginning, there was much more access to publicly accessible testing centers, for free,” said Brian Sasser, chief communications officer at the Episcopal Health Foundation. “Obviously, that was beneficial to everyone, especially those without insurance.”
But if testing requires paying out of pocket or visiting a doctor, Sasser said, many people without insurance just won’t get tested. That’s particularly true for people who work at jobs that don’t offer them paid time off or insurance.
“It’s one of those reinforcing loops where it’s tougher to get a test, and also there’s less incentive to get a test, because if you find out you’re positive, you don’t get paid for work,” he said. “The end result is people are put at risk … and could be potentially putting other people at risk. It all becomes the perfect storm.”
Sasser hopes the pandemic has underscored the fragility of a health insurance system that is tied to employment and, often, only full-time professional work. By May 2020, just two months into the pandemic, more than 650,000 Texans were estimated to have lost their employer-sponsored health insurance.
Lagging vaccination rates
Among the most pressing questions for health care workers right now is how effective COVID-19 vaccines are against the omicron strain — and how to get more vaccines and boosters into the community. In El Paso County, 65% of residents are fully vaccinated, about 10 percentage points higher than statewide. Salazar, with La Fe, said getting those shots into arms has required a lot of work.
“The most important part is the outreach: knocking on doors, letting people know that we’re there, letting people know that we are not requiring insurance and not even requiring paperwork other than identification so that we can get everybody immunized,” he said.
Coronavirus vaccines and booster shots are free, regardless of whether a patient has insurance. Texas doesn’t track the insurance status of vaccinated individuals, but a national survey from the Kaiser Family Foundation in September found uninsured adults were lagging significantly behind on vaccination.
Health care workers who serve uninsured patients say they hear concerns about hidden costs, like side effects that would require medical care. Or, they worry, people without insurance might not have trusted medical professionals they can ask for advice.
And in border communities like El Paso, Salazar said, they’re fighting against a rising tide of government mistrust. He said Gov. Greg Abbott and former President Donald Trump have stoked fears about immigration enforcement in heavily Latino communities.
“Then, all of a sudden, they’re saying we have to get immunized, and we’re starting to see some of these ghosts of past lack of trust come up,” he said.
“Put on the shoes of the immigrant that’s a front-line worker that can’t speak the language, that lives in a colonia, that has to work to survive, and at the same time, might have somebody in their home that doesn’t have all the right paperwork,” he said.
Salazar said these personal circumstances, plus rising anti-immigration rhetoric and enforcement, are a “volatile combination” of forces that discourage people in the area from seeking public services, including vaccines.
This fear isn’t limited to the border. In other parts of the state, Black leaders have mobilized to address vaccine hesitancy that stems from mistrust of government and health care systems that are often adversarial to Black patients. There were also concerns early on that Black and Hispanic communities were not getting equal access to vaccination sites.
While Hispanic people are now getting vaccinated at slightly higher rates than whites in Texas, Black people continue to have the lowest vaccination rates in the state.
This article was originally posted on Texas has the highest share of uninsured residents in the nation. Another COVID-19 wave puts them at risk.